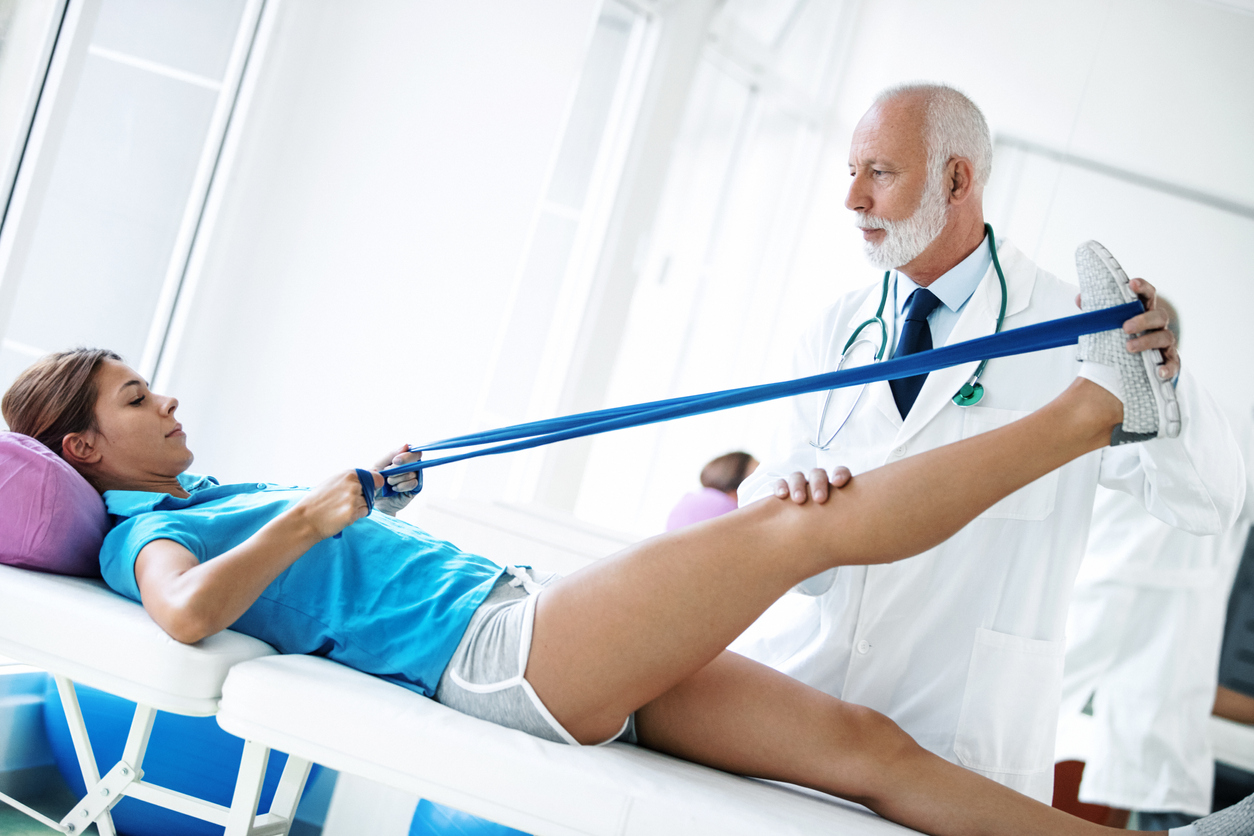
There are many reasons to become an orthopedic sports medicine surgeon. This specialty includes high volume surgical techniques, evidence-based care and disease management. Students can interact with physicians in other disciplines through weekly multidisciplinary conferences. This gives students the chance to gain first-hand knowledge about sports injuries and other conditions. Read on to learn more about the field of orthopedics and become a surgeon. Listed below are some of the benefits of becoming an orthopedic sports medicine surgeon.
Common musculoskeletal injuries
Musculoskeletal disorders (MSDs) are highly prevalent in the United States and cause severe pain and mobility loss in over 10 million people each year. They are responsible for a significant portion of the total number of days lost due to absence from work, and they also have long-term consequences. There are both nonsurgical and surgical treatments available for these injuries, and recovery times can be lengthy, with some injuries never returning to pre-injury levels.
In addition to orthopedic sports medicine, physical therapy also has a role in treating common musculoskeletal injuries. Soft tissue injuries can be treated using rest, ice, compression, elevation, and other techniques. Follow-up with an expert in pediatric or adolescent sports medicine is essential for establishing the proper diagnosis and initiating treatment. In rare cases, an orthopedic referral may be necessary.
Treatment options
Nonoperative treatment options in orthopedic sports medicine include stem cell injections. These cells can be derived from healthy areas of the body and injected into the injured area, promoting healing without surgery. Another treatment option is called perineural superficial injections, which target inflamed nerves. These injections can alleviate pain and spasms and increase mobility. However, patients should be wary of their risks before undergoing this treatment.
A doctor specializing in orthopedic sports medicine may perform surgery on patients who need it. Depending on the severity of the condition, the physician may recommend surgery to repair the affected part. Surgical options include arthroscopy, bone grafts, and joint replacement. Orthopedic surgeons also perform procedures for patients who are unable to undergo other types of treatment. Orthopedic sports medicine doctors specialize in treating both acute and chronic conditions.
Certification requirements
Before pursuing a career in orthopedic sports medicine, doctors should earn a General Certificate in Orthopedic Surgery. This certificate is good for 10 years, during which time they can apply for subspecialty certificates. Orthopedic sports medicine is one of these subspecialties, and obtaining it requires that the physician meet certain practice requirements. There are two parts to the certification exam: a computer-based portion and an oral component. Physicians who fail the computer exam must take it again.
The first step in the path to becoming a sports medicine physician is to earn a medical degree. Physicians seeking to become primary care sports medicine physicians typically complete a three-year residency in family medicine, emergency medicine, and neuromusculoskeletal surgery. Those aspiring to become orthopedic surgeons complete an orthopedic surgery residency. However, physicians interested in primary care sports medicine can earn a certificate in either specialty.
Research in the field
There are many different areas of research in the field of orthopedic sports medicine. The topics covered range from basic science to more advanced areas. For example, research in the field of sports medicine focuses on rehabilitation after injury and rehabilitation of the musculoskeletal system. This includes identifying the key pathways in muscle repair, inflammation, regeneration, and fibrosis. The aim of these research initiatives is to address the increasing burden of orthopedic diseases on our society.
FDs are also influential in the future of orthopedic trainees, yet little is known about their demographics. Furthermore, there is little information available on the training and academic background of current FDs in sports medicine. The study findings may help promote future research on leadership in the field of orthopedic sports medicine. Further, the study will provide a demographic profile of current sports medicine FDs. FDs are critical leaders in the field, and this study will provide a baseline for assessing future leadership in the field.











